Incontinentia pigmenti treatment is symptomatic and supportive. There is currently no cure for IP.
For infants and children, parents should engage a team of physicians to address the numerous features of the spectrum of IP. Preferably, these approaches should be guided by and supported by a geneticist familiar with the condition and its manifestations. The team may include a pediatric ophthalmologist and/or a pediatric retinal specialist, a neurologist, dermatologist, and eventually a pediatric dentist. Each specialist should determine what is in the child’s best interest for incontinentia pigmenti treatment depending on appropriate testing, including sedations of any kind.
One summary may be found here: National Protocol for the Diagnosis and Care of Rare Diseases: Incontinentia Pigmenti. For additional recommendations, jump to:
Eyes
Recommended Specialists – Pediatric Ophthalmologist and/or Retinal Disease Specialist, Ophthalmologist
Required Eye Examinations
It is imperative to have a complete medical eye examination as soon as possible after diagnosis.
A dilated retinal examination as soon after birth as the neonatologist or anesthesiologist thinks is safe. Sometimes, if there are any suspected retinal blood vessel abnormalities, an examination under anesthesia is required. The important thing is for the ophthalmologist to look at the optic nerve, the macula (in the center of the retina), and the far peripheral retina, where the typical pathologic events tend to occur. Do this before the baby leaves the hospital.
A fluorescein angiogram is highly recommended, regardless of age, initially and at follow-up. unless the retinal specialist decides the view of the retina is easily and completely obtainable without the angiogram. An angiogram will help the physician see the vessels located in the periphery of the eye where bleeding can occur and which cannot be seen by the naked eye.
The retinal specialist will determine how frequently to repeat the examinations and the angiograms depending on retinal findings obtained with routine examination techniques. As our technology evolves and the camera systems change, newer approaches to imaging may replace fluorescein angiography, including Ocular Coherence Tomographic Angiography (OCT-A).
These examinations and imaging systems are looking for serious abnormalities in the growth and development of the small blood vessels that nourish the retina, similar to those that occur in very low birth weight premature babies, called “Retinopathy of Prematurity”. Discovery of these changes requires monitoring for the further development of abnormal blood vessels, new blood vessel growths, and bleeding that results from them, which would then require treatment with laser or freezing therapies to obliterate the abnormalities to salvage the retina from further damage.
Severe retinal blood vessel disease is sometimes associated with blood vessel damage in the brain and thus is a marker to pursue imaging studies of the head. With respect to the eyes themselves, some babies with IP, and even some older patients, might benefit from laser treatment in an effort to prevent retinal detachment or vitreous hemorrhage from the consequences of the typical retinal neovascularization that occurs in this disorder.
Recommended Schedule
If eyes are normal at the initial full IP eye examination and thereafter, eye appointments with dilation follow-ups should be scheduled monthly until age four months. After that, schedule examinations approximately every three months or so from age four months to one year; every six months from age one to three years; and annually after age three years until the mid-teen years.
If an important issue or question should arise at any time during an examination, immediately see a retinal specialist or pediatric ophthalmologist and refer back to the full ophthalmologic examination thereafter.
If any eye or head trauma occurs at any time throughout life, get an ophthalmic examination as soon as possible to rule out partial or full retinal detachment.
Additional Guidelines
Most IP persons have normal vision (with corrective lenses). Some problems, like near- and far- sightedness, are common in persons with IP. But, these are probably no more frequent than the general population without IP.
The classical eye finding in IP is an abnormality in the growth and development of blood vessels in the inside of the eye (the retina). Growth of abnormal blood vessels and the associated scarring can cause loss of vision, but can be treated if recognized early enough.
For this reason, babies diagnosed with IP should have the full IP eye examination immediately after birth and be followed by an ophthalmologist closely. Have a pediatric ophthalmologist or retinal disease specialist conduct a careful examination
In some older literature, some eye abnormalities have been reported, such as small eye (microphthalmos), cataract, degeneration of the optic nerve (optic atrophy) and even or total blindness. However, these complications occurred in an era before the retinal blood vessel abnormalities were recognized and were treated in the more recent times. However, a cataract is never a primary feature of IP and occurs only after substantial damage has occurred to the retina inside the eye.
If you are a pregnant woman with IP who had eye abnormalities, talk with your eye doctor. You may need a different way to deliver your baby for the safety of your eyesight.
Brain
Recommended Specialist – Neurologist
A neurologist is a physician who specializes in understanding the brain and its function. The brain is extremely complex, and disorders within the brain or nervous system can alter behavior and cognitive function.
We suggest a baseline magnetic resonance imaging (MRI) or magnetic resonance angiography (MRA) test with and without contrast as soon as reasonable after birth or diagnosis, especially if the retinal blood vessels are abnormal by observations.
IP can be associated with learning disabilities. If your school-age child has delays or hardships despite a high IQ, have a neuro psychological exam. This will help you and educators at your school implement an individualized education program (IEP) so your child receives appropriate assistance.
Seizures or other complications should be treated as in any other infants.
Pulmonary
Recommended Specialist – Pulmonologist
IP can be associated with pulmonary hypertension. Have a non-evasive baseline test at birth and monitor closely for the first year of life. The suggested timeline is birth, three months, six months, nine months, and one year.
Genetics
Recommended Specialist – Geneticist
A geneticist should be and often is a family’s IP team leader for care throughout life, including follow-ups at the developmental milestones: pre-natal, all IP births, and puberty.
Molecular genetic (DNA) testing with or without skin biopsy is required for specific diagnosis of IP. Visit the CDC website for additional information on genetic testing and links to genetics experts.
Skin and Hair
Recommended Specialist – Dermatologist
A baby affected by IP should be watched carefully by a pediatric dermatologist for the first year of life.
Keep the skin cool and dry during all stages for the first year. It is imperative to avoid secondary infection. If it occurs, treat the secondary infection from common skin bacteria.
All stages of the skin may overlap one another for the first year of life and stages may repeat themselves. Each infant is different in severity and longevity. There is no “cure” for the skin stages. They will run their course for each case.
Associated with the scarring of the skin in IP, some people have had problems with heat intolerance and lack of sweating. If this is a concern, discuss this with your dermatologist. You can also download our Cooling Guide.
Teeth
Recommended Specialists – Pediatric Dentist, Dentist, Orthodontist, Oral Surgeon, Periodontist, Oral and Maxillofacial Surgeon
Recommended Dental Visits
Dental health is an important part of incontinentia pigmenti treatment. Routine dental care should be started by approximately 6 months of age to help prevent the likelihood of developing tooth decay and to begin evaluating the presence/absence of teeth. Dental development is monitored and preventive measures applied through early childhood. If missing and or malformed teeth are an esthetic issue for the child, treatment can be considered to help the child maintain a positive self-image.
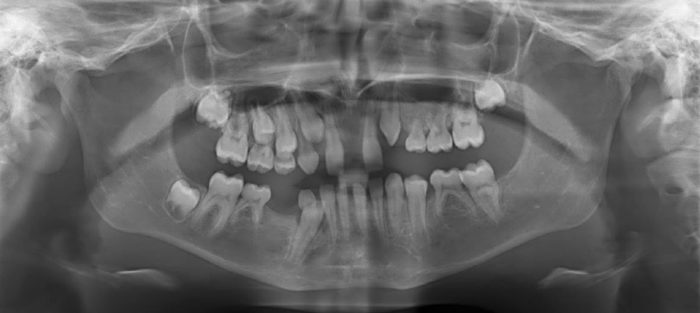
Missing and malformed teeth can be challenging to manage depending on several factors, such as, the number of teeth missing, the shape and location of the teeth present and the presence of tooth mal-alignment to mention just a few. Treatment may consist of bonding and crowns to reshape teeth, fixed or removable dentures or bridges to replacing missing teeth and implants. Orthodontics is commonly used to align teeth. A team approach is often best to manage these different oral issues and to help coordinate and time treatments optimally.