
SYNONYMS
- Bloch-Sulzberger syndrome
- Bloch-Siemens incontinentia pigmenti
- Pigmented dermatosis Siemens-Bloch type
Incontinentia pigmenti (IP) is an X-linked dominant disorder and in males, is usually lethal before birth. In affected females, it causes highly variable abnormalities of the skin, hair, nails, teeth, eyes, and central nervous system.
Incontinentia Pigmenti (IP Syndrome) is a Rare Genetic Condition Characterized by
Skin
There are four incontinentia pigmenti stages for skin manifestations, which may overlap. The earliest and most striking diagnostic features in IP occur in the skin are progressive rashes.
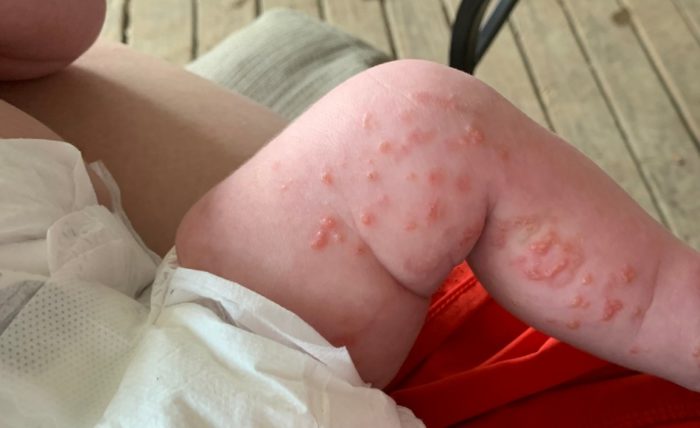
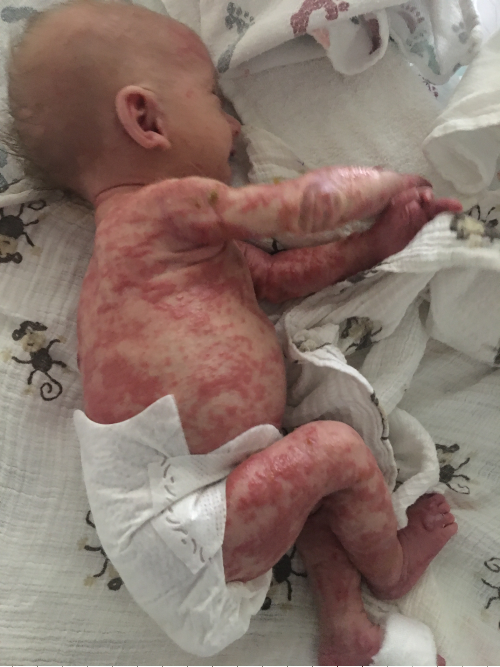
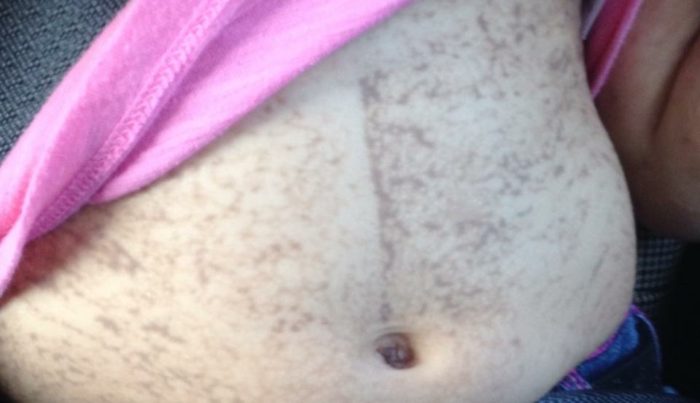
Minor Criteria: Occur, but Not Necessary for Diagnosis
Growth
- Short stature in adolescence and adulthood
Head
- Microcephaly in cases of severe intracranial damage during pregnancy and infancy
Eyes
- Microphthalmos, a small eye if there is severe retinal blood vessel damage in infancy
- Strabismus, or crossed eyes, typically in situations of early onset retinal bleeding and consequent damage
- Abnormal retinal blood vessel formation and retinal bleeding in infancy, leading to new blood vessel formations, and potentially retinal scarring and membrane formation and, in the extreme, tractional retinal detachment.
- Foveal (central vision area of the retina) underdevelopment or disorganization
- Abnormally small eyes (if the retinal damage is extensive and leads to total retinal detachment early in life)
- Retinal vascular proliferation (some of the vessels carrying blood to or from the retina become blocked or do not carry blood normally). The retina is the inner coat of the eye which is a light-sensitive layer of tissue.
- Optic atrophy (the loss of some or most of the nerve fibers in the optic nerve, if the retinal vascular disease is severe and early onset). The effects range from visual changes to severe visual loss.
- Eyes do not properly align with each other as a secondary event following poor vision when the retinal damage is severe (strabismus)
- Retinal bleeding from the abnormally formed blood vessels in early life
- Formation of excess fibrous tissue on the retinal surface (retinal fibrosis)
- Separation of the retina from its attachments to the underlying tissue within the eye (retinal detachment) caused by the scarring after the growth of extensive new blood vessel formation in some females
- Abnormality of the center part of the retina (foveal hypoplasia) if the blood flow and capillary development in that zone is damaged early in life
Teeth

- Fewer than the normal number of teeth (hypodontia)
- Delayed eruption
- Wide spacing between teeth (diastema)
- Cone shaped teeth, particularly incisors
- Accessory points on the surface of some teeth
More than 80% of IP patients have abnormalities of their teeth. This can be useful in making the diagnosis of IP. The primary (baby) teeth may be delayed. Both the baby and adult teeth may be affected. Adult teeth can be affected even when baby teeth have been normal.
Ribs Sternum Clavicles & Scapulae
- Extra ribs have been described infrequently
Breasts
- Extra (supernumerary) nipples
- Nipple hypoplasia
- Small breast development at puberty
- Asymmetric breast development after puberty
- Complete lack of breast development (rare)
Spine
- A type of vertebral anomaly that results from a lack of formation of one half of a vertebral body. It can be a common cause of early onset scoliosis. (hemivertebrae)
- A combination of outward curvature (kyphosis) and lateral curvature (scoliosis) of the spine (kyphoscoliosis)
Nails
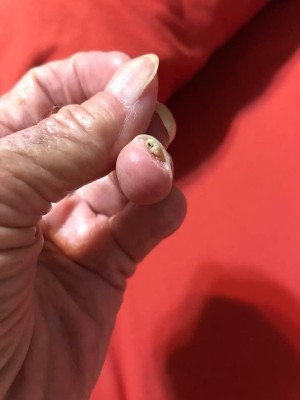
- Lose shape or are partially or completely damaged (nail dystrophy)
- Ridging
- Pitting
- Tumors (usually benign but occasionally painful) under the nail bed (subungual keratotic tumors)
- Thickening that may produce nails resembling claws or a ram’s horn (onychogryphosis; also known as ram’s horn nails)
IP can affect the nails of both the hands and feet. Abnormalities are usually mild and transient but can recur. They typically involve most or all fingernails and toenails, not just one or two nails.
Benign tumors can grow under the nail bed and correspond with the blistering skin lesions seen in Stage 2. In extreme cases, these growths can be painful and may be associated with deformities of the finger bones or nail beds.
Hair
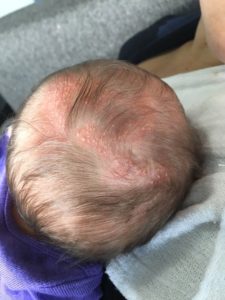
- Patchy alopecia and hair loss (vertex/ crown of head) following the scarring of the skin when the scalp blisters heal
- Wiry, coarse hair in childhood
- Thin, sparse hair in childhood
Approximately 50% of women with IP have minor abnormalities of their hair, typically a loss or lack of hair (alopecia) on the crown of the head. Scarring from the rash probably causes the alopecia, but this is not proven. Sparseness of hair as a child does not correlate with the quantity of hair as an adult.
Central Nervous System
- Seizures usually following a history of intracranial bleeding in infancy
- Stroke-like episodes in the first few months of life
- Intellectual disability, especially following severe intracranial bleeding in infancy
- Spasticity (unusual “tightness”, stiffness, or “pull” of muscles.) or “cerebral palsy”
Although most affected individuals are neurologically normal, IP can cause severe neurologic complications starting in infancy. Abnormalities of the nervous system can include seizures (epilepsy) in infancy. Paralysis, developmental and intellectual impairment, and small head size in infancy are possible and seem to result from damage to the blood vessels in the brain in early postnatal development. There is increasing evidence that, if problems are going to arise, they will appear within the first year of life.
Hematology
- Leukocytosis with hypereosinophilia during stage 1
DIAGNOSING INCONTINENTIA PIGMENTI
A physician may suspect incontinentia pigmenti (IP) in an infant on the basis of physical features, especially if the mother has a formal diagnosis of IP. However, in the isolated case, the skin manifestations are often mistaken for a viral rash (such as chicken pox, herpes impetigo or scabies) and the baby is placed in isolation and treated with antiviral drugs until either a skin biopsy or preferably a genetic test confirms the correct diagnosis.
If the classic rash is present in a newborn, the diagnosis is straightforward. But, it can be more difficult when the rash is mild, when not all the stages are present because Stage 1 and even Stage 2 may have occurred in the womb, or when an adult is seen and the streaky skin lesions have faded. A skin biopsy that shows the presence of “loose” melanin (the brown-black skin pigment) in the dermis of the skin strongly implies the diagnosis, in the appropriate clinical setting, but molecular genetic testing is the most accurate and readily available procedure to secure a firm diagnosis.
When there is little or no skin involvement, IP may be assumed to be the diagnosis in individuals “at risk” for the condition if they have other features, such as tooth abnormalities (after the teeth begin to develop and erupt), missing patches of hair, or overgrowth and scarring of the retinal blood vessels. Such an “at risk” individual would be a woman with two (or more) affected daughters, the daughter of an affected woman, or the sister of an affected woman who herself has had the miscarriage of more than one male fetus.
Diagnostic Criteria for the Disorder
Major criteria including any of the four stages of skin lesions described by Landy and Donnai (1993), and minor criteria including dental, ocular, central nervous system, hair, nail, palate, breast, and nipple anomalies, as well as the history of multiple male miscarriages (typically before 12 weeks, but as late as 20 weeks, gestation) in the affected mother, the histopathologic skin findings at biopsy, or preferably the molecular confirmation for the causal gene.
Cause of Incontinentia Pigmenti
Mutations in the IKBKG gene, also called NEMO, that is located on the X-chromosome cause IP. The gene for IP was identified in 2000 by collaborations of some members of the Scientific Advisory Council of the NFED.
The protein produced by this gene is important in regulating the nuclear factor-kappa-B (NFKB) pathway. This is the same pathway involved in several ectodermal dysplasias including the X-linked hypohidrotic form.
Genetic Testing
Testing is available for IP both to confirm the diagnosis in a female with the clinical features and in an at-risk fetal pregnancy by the usual mechanisms of chorionic villus sampling, amniocentesis.
IP Inheritance
IP is inherited as an X-linked dominant “lethal” condition. An IP-affected female has three possible outcomes at the birth of any pregnancy with equal probability: an unaffected female, an affected female, and an unaffected male. Since the affected male conception dies in the womb, affected males do not survive to the usual birth and are not seen in this situation.
Females
If the pregnancy is a female (who thus inherits her other X-chromosome from her father), that child will be a female who has two normal X-chromosomes and is unaffected.
If the affected female passes on the X-chromosome with the abnormal NEMO gene on it and her male partner passes on his X-chromosome, that child will have two X-chromosomes and thus be female, but since one X-chromosome has the abnormal gene, that female will be affected with IP.
Males

If the mother passes on her normal X-chromosome and her partner passes his Y-chromosome, that child will be XY, and this a male. His only X-chromosome is the normal copy and he will be unaffected.
If the affected female passes on her X-chromosome with the abnormal NEMO gene and her partner passes on his Y-chromosome, that child will be XY and a male. His only X-chromosome has the causal mutation on it. That male will develop IP and typically dies in the womb at about 12 weeks of pregnancy (sometimes later).
In an extremely rare case, a normal unaffected mother may give birth to an affected male child if some of his cells changed or mutated the NEMO gene after his conception, making him a mosaic. If he survives to adulthood, rare cases of transmission of IP from a mosaic father to an affected female have been documented with molecular confirmation.
Affected Population
There is no known ethnic or racial predisposition. The prevalence of IP is unknown. As often with rare disorders, it is likely that IP is often undiagnosed or misdiagnosed.
IP TREATMENT
While there is no known cure for incontinentia pigmenti (IP), there are treatment protocols and recommended medical specialists for affected areas of the body like skin, hair, eyes and more.
LEARN MORE ABOUT IP
- Online Mendelian Inheritance in Man
- GeneReviews
- Incontinentia pigmenti: Report on Data from 2000-2013
FAMILY PERSPECTIVES
- Guatemalan Family Fights to Save Their Baby
- Read Lacy Light’s story in this article: What You Need to Know To Help Your Child’s Vision if They Have IP